11/15/2010
Previous | Next | Health Home | Career Corner | Issues | Personal Finance
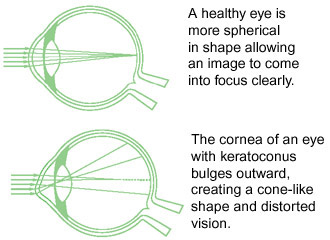
Keratoconus is a progressive eye disease in which the normally spherical cornea thins and begins to bulge into a cone-like shape. The cornea is the clear, central part of the surface of the eye. In patients with keratoconus, the cone-shaped cornea cannot focus light rays properly and causes distorted vision.
Causes of Keratoconus
Although many theories have been proposed, there is no one definite known cause of keratoconus. Possible etiologies include genetics, a collagen deficiency, and excessive eye-rubbing.
Sign and symptoms of Keratoconus
Keratoconus often begins to develop in the teen years to the early 20s, although it can develop at any age. Changes in the shape of the cornea occur gradually, usually over several years. In most patients with keratoconus, both eyes eventually become affected.
Keratoconus can be difficult to detect because it usually develops very slowly. Signs of keratoconus may include:
-- Distorted and blurred vision
-- Myopia (nearsightedness
-- Astigmatism
-- Double vision
-- Headaches due to eye strain
-- Glare
-- Light sensitivity
Your doctor will measure the curvature of your cornea to determine whether these symptoms are a result of keratoconus.
Treatment for Keratoconus
In the early stages of keratoconus, glasses or soft contact lenses may correct the nearsightedness and astigmatism associated with the disease. As the condition progresses and the cornea becomes increasingly thin, more advanced treatment is required
Rigid Gas-Permeable Contact Lenses: If eyeglasses or regular soft contact lenses cannot control keratoconus, rigid gas-permeable (RGP) contact lenses are usually the preferred treatment. The rigid lens covers the cornea, replacing the cornea's irregular shape with a smooth, uniform refracting surface, improving vision.
Rigid contact lenses can be less comfortable to wear than soft lenses. Further, fitting contact lenses on a cornea with keratoconus can be challenging and time-consuming. If you are using RGP contact lenses, you will need to visit your doctor frequently to fine-tune the fit and prescription of the lenses, especially if your keratoconus continues to progress.
Intacs®: Intacs are plastic rings inserted into the mid-layer of the cornea to flatten it, changing the shape and location of the cone. INTACS may be needed when distorted vision from keratoconus can no longer be corrected with contact lenses or eyeglasses. The implants are removable and exchangeable. If keratoconus continues to progress, however, Intacs can only delay the need for a corneal transplant, not prevent it.
Collagen Cross-Linking: Collagen cross-linking is a relatively new method for treating keratoconus. It works by strengthening the corneal tissue to stop it from bulging. In this procedure, eye drops containing riboflavin (vitamin B2) are applied to the cornea and then activated by ultraviolet light. This strengthens the collagen fibers within the cornea. This procedure is not yet FDA approved.
Corneal Transplant Surgery: Surgery is needed for patients with advanced keratoconus, if scarring has occurred. This treatment may be recommended for 15-20% of cases. In corneal transplant surgery, most of the cornea is removed and then replaced with a new donor cornea. The results of the procedure have a success rate of over 97%.
More on Intacs treatment
Intacs® corneal implants are clear, thin half-rings used to correct corneal astigmatism and myopia (near-sightedness). They are placed in the peripheral cornea and work from within to reshape and support the cornea. Intacs are most often used to treat keratoconus, a degeneration that causes corneal weakening and thinning, resulting in myopia and astigmatism.
Intacs implantation is a relatively low risk procedure. The implants do not weaken the cornea like LASIK or PRK (which are contraindicated in keratoconus) because no corneal tissue is removed. The short procedure (15 to 20 minutes) takes place in a LASIK suite and utilizes the same laser used in LASIK (Femtosecond laser). Numbing drops are administered, and the Femotsecond laser creates two corneal tunnels for the Intacs rings.
Recovery can be expected within a day or two and the full healing process takes approximately one month. Many patients no longer depend on glasses or contact lenses after the procedure. There is no post-operative maintenance and the implants cannot be felt or seen. They can be removed or replaced for new prescriptions.
Intacs are FDA-approved for people with keratoconus who are at least 21 years old and unable to tolerate contact lenses or glasses. They are an exciting option for individuals experiencing intolerance to contact lenses and are facing a corneal transplant. Intacs corneal implants may be the best possible option to restore comfortable contact lens wear, improve vision, and potentially postpone the need for a corneal transplant. Complications from the Intacs procedure are rare, but can include infection, glare, halos and fluctuating vision.
Mark D. Fromer, M.D., board certified ophthalmologist in surgery and treatment of eye diseases, has the distinction of being the eye surgeon for the New York Rangers hockey team. Dr. Fromer specializes in laser vision correction procedures, lectures extensively throughout the U.S., and maintains a very active role in teaching advanced surgical techniques and laser vision correction surgery to fellow ophthalmologists. Maayan Keshet, M.D., a board-certified cornea and external disease specialist, is an Assistant Attending Physician and Instructor at NY's St. Luke’s-Roosevelt Medical Center where she supervises residents in cornea and cataract surgeries and leads weekly discussions on cornea topics. Fromer Eye Centers, with three offices in NYC, is one of only four beta sites worldwide for the latest diagnostic software developed by Heidelberg instruments for the early detection and treatment of diabetic macular edema. For more information on this and other forms of advanced vision care, visit Fromer Eye Centers.
© 2010 Dr. Mark FromerThe views and opinions expressed in these articles do not necessarily reflect those of College Central Network, Inc. or its affiliates. Reference to any company, organization, product, or service does not constitute endorsement by College Central Network, Inc., its affiliates or associated companies. The information provided is not intended to replace the advice or guidance of your legal, financial, or medical professional.